This article collects the best answers to Georgia’s Medicaid’s most frequently asked questions.
Medicaid is a government-sponsored healthcare program for low-income families and individuals who fulfill specific income and resource requirements. Only the aged, blind, or disabled can access resources within the defined restrictions.
We have scoured the internet to provide all you need to know about the Georgia Medicaid Benefits.
You will learn everything you need to know about Georgia Medicaid in this article.
Table of Contents
What is Georgia Medicaid?
Georgia Medicaid, also known as the Georgia Medical Assistance program, is a federal and Georgia-state funded health care program for those in financial need.
Similar Articles:
- How to Get Hawaii Medicaid Benefits | Best Answers
- How to Get Indiana Medicaid Benefits | Best Answers
- How to Get Iowa Medicaid Benefits | Best Answers
Who is eligible for Georgia Medicaid?
You must be a resident of Georgia, a national or citizen of the United States, a permanent resident, or a legal alien in need of health care or insurance help, and have a low income to qualify for Georgia Medicaid. You must also be one of the following:
- Pregnant, or
- Be in charge of a child who is younger than 18 years old, or
- Having a disability or residing with a family member who does
- Be 65 years of age or older.
Annual Household Income Limits (before taxes)
| Household Size* | Maximum Income Level (Per Year) |
| 1 | $33,568 |
| 2 | $45,226 |
| 3 | $56,885 |
| 4 | $68,543 |
| 5 | $80,201 |
| 6 | $91,860 |
| 7 | $103,518 |
| 8 | $115,177 |
*For households with more than eight members, add $11,659 per additional person.
How do I contact Medicaid in Georgia?
Phone
877-423-4746
https://dch.georgia.gov/contact-dch
Website
How do I apply for Georgia Medicaid?
Visit the Georgia Gateway online application portal to apply.
Visit the Applying for Medicaid page for more information on the application process. An application form will be available for direct download from the website.
Additionally, you can use the Marketplace application to see whether you are eligible.
What are the Medicaid plans in Georgia?
Three national, for-profit health plans (WellCare, Peach State Health Plan, and Amerigroup Community Care) have contracts with Georgia to provide services in at least three of the state’s six designated geographic districts.
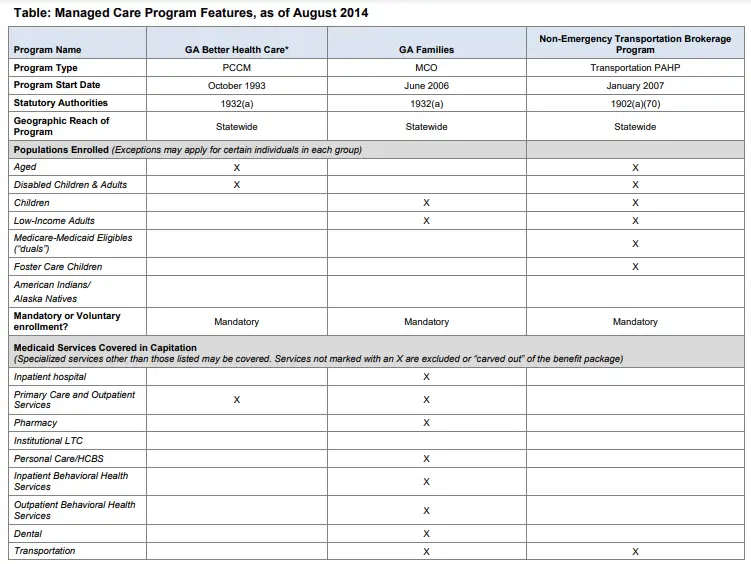
- Georgia Better Health Care is the initial PCCM initiative of the state. The current Medicaid managed care organization (MCO) program, Georgia Families, offers primary, urgent, and specialty care and dental, behavioral health, and transportation services.
- The majority of Medicaid recipients in the state, including those not signed up for Georgia Families, are provided with transportation services on a mandated basis through the Non-Emergency Transportation Brokerage Program.
- Medicaid recipients who are elderly or disabled and need nursing home care can enroll in the SOURCE (Service Options Using Resources in a Community Environment) program and work with a primary care physician who will coordinate general medical care, specialized care, and home and community-based services.
Similar Articles:
- How to Get Kansas Medicaid Benefits | Best Answers
- How to Get Louisiana Medicaid Benefits
- How to Get Maine Medicaid Benefits
What is covered by Georgia Medicaid?
The following services are covered by Georgia Medicaid
| Certain emergency dental care for adults | Laboratory services |
| Diagnostic and screening services | Medical equipment and supplies |
| Doctor and nurse office visits | Mental health clinic services |
| Emergency ambulance services | Non-emergency transportation |
| Exams and vaccines for children | Nurse midwife |
| Family planning services | Nursing facilities |
| Hearing services for children | Prescription drugs |
| Hospice care services | Preventive dental care for children |
| Hospital services | Vision care for children (limited for adults) |
Copayments?
| Ambulatory surgical centers/birthing | $3.00 |
| Durable medical equipment | $2.00 |
| Federally Qualified Health Centers | $2.00 |
| Free-Standing Rural Health Clinic | $2.00 |
| Home health services | $3.00 |
| Hospital-Based Rural Health Center | $2.00 |
| Inpatient hospital services | $12.50 |
| Oral maxillofacial surgery | Cost-Based |
| Orthotics and prosthetics | $3.00 |
| Outpatient hospital services | $3.00 |
| Pharmacy – preferred drugs | $0.50 |
| Pharmacy – non-preferred drugs | Cost-Based |
| Physician assistant services | Cost-Based |
| Physician services | Cost-Based |
| Podiatry | Cost-Based |
| Eye care | Cost-Based |
Which Medicaid members do not have to pay copayments?
The following Georgia Medicaid participants are exempt from making copayments:
- Medicaid members under the age of 21
- Pregnant women
- Members with breast and cervical cancer
- Members in nursing homes
- Members of hospice care
- American Indians
- Alaskan natives
Can I have both Georgia Medicaid and Medicare?
An individual may be qualified for both Medicaid and Medicare and be able to use both programs simultaneously. People must be enrolled in Medicare Part A (hospital insurance) and Medicare Part B to be considered dual-eligible (medical insurance).
What is the highest income limit for Georgia Medicaid?
The highest income limit for Georgia Medicaid for an individual is $2,135 per month.
Which is the best Medicaid plan in Georgia?
Georgia’s top-rated Medicaid plan for customer satisfaction is WellCare.
Will you still have Georgia Medicaid once you are over 18?
From the time a child is born until the final day of the month in which the youngster is nineteen (19), RSM for Children covers their medical expenses. Depending on their age, family size, and income, these kids may qualify at various income levels.
How much money can you have in the bank on Georgia Medicaid?
When people apply for Medicaid for long-term care in Georgia, they can keep $2,000 of their income. The Medicaid asset cap only applies to countable assets, which might vary in size depending on factors including the applicant’s spouse’s Medicaid need.
Similar Articles:
- How to Get Maryland Medicaid Benefits
- How to Get Massachusetts Medicaid Benefits
- How to Get Michigan Medicaid Benefits
Does the disabled person get Georgia Medicaid?
Millions of Americans, including kids, expectant mothers, parents, retirees, and those with disabilities, have access to health coverage through Medicaid.
ABD MEDICAID IN GEORGIA: In Georgia, ABD Medicaid is available to anyone 65 years of age or older who is also totally disabled. The ABD population has 19 distinct coverage categories or classes of assistance (COA).
What documents do I need to apply for Medicaid?
Following documents must be included with the application:
- Social Security Number;
- Proof of Identity (driver’s license);
- Proof of Citizenship (birth certificate);
- Health Insurance;
- pregnancy (doctors’ confirmation of the pregnancy and the anticipated delivery date, if any);
- Income of Non-pregnant parents applying for Medicaid for themselves should bring proof of resources (last three months’ bank statements, checking or savings account information, life insurance policies, stocks, and bonds).
