We have scoured the internet to provide all you need to know about the Montana Medicaid Benefits.
Medicaid is a joint federal-state initiative that covers healthiness for low-income persons who qualify, including children, households, pregnant women, the elderly, and people with disabilities. It is simple to apply for Medicaid in person, over the phone, or online.
This post will teach you all you need to learn about Medicaid in Montana.
Table of Contents
What is Montana Medicaid?
Medicaid is a service for people and families with income and resources that fall inside certain parameters. Resources primarily apply to the elderly, blind, or disabled population within the bounds of specified rules.
Who is eligible for the Montana Medicaid Program?
Montana Medicaid offers limited Medicare beneficiaries who are not eligible for the entire Medicaid benefit package partial financial help with Medicare premiums, copayments, or coinsurance through the Medicare Savings Plan.
- Expectant mothers
- People who are blind or disabled or who have a spouse who is blind or disabled;
- People whom someone adopts;
- People whom someone adopted;
- People who are blind or disabled or have a spouse who is disabled.
Annual Household Income Limits (before taxes)
| Household Size* | Maximum Income Level (Per Year) |
| 1 | $13,590 |
| 2 | $18,310 |
| 3 | $23,030 |
| 4 | $27,750 |
| 5 | $32,470 |
| 6 | $37,190 |
| 7 | $41,910 |
| 8 | $46,630 |
* Add $4,720 for every extra member in families with 9 or more inhabitants.
Similar Articles:
- How to Get New Hampshire Medicaid Benefits?
- How to Get New Jersey Medicaid Benefits?
- How to Get New Mexico Medicaid Benefits?
How do I contact Medicaid in Montana ?
Phone
1 (800) 362-8312
Mailing Address
Montana Department of Public Health and Human Services
1400 Broadway PO Box 8005
Helena, MT 59604
Website: https://dphhs.mt.gov/
What are the Medicaid plans in Montana?
Following are the medicaid plans in Montana:
- Montana Living Life Well Program
- HMK (Healthy Montana Kids)
- Montana HELP Plan
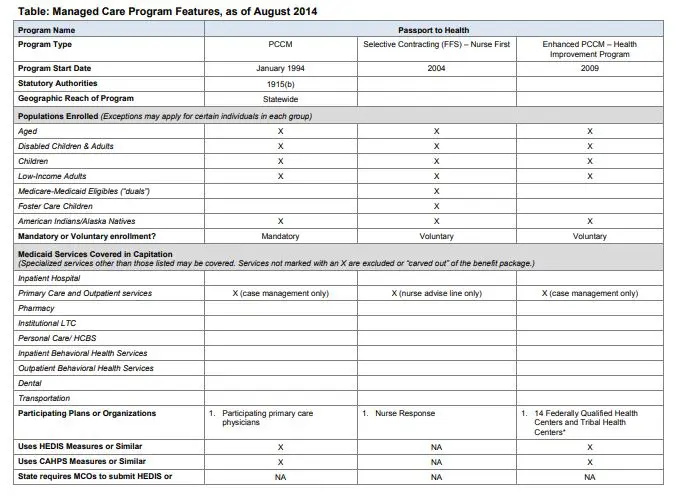
- Montana Medicaid Passport to Health
How do I apply for Montana Medicaid?
Online: Montana.gov
Call: 1-800-318-2596
In Person: Visit your local community health center or local Office of Public Assistance.
Can I have both Montana Medicaid and Medicare?
Medicare and Medicaid are available to those 65 years old or older. If your age is below 65, you can only avail of the benefits of Medicaid if other eligibility criteria are fulfilled.
What is covered by Montana Medicaid?
The following services are covered by Montana Medicaid:
| Ambulatory surgery | Hospital stays |
| Audiology services | Laboratory tests |
| Behavioral health services | Maternity care |
| Dental services | Non-emergency transportation |
| Dialysis | Orthotic and prosthetic devices |
| Doctor visits | Women’s health care |
| Durable medical equipment | Pharmacy (medications) |
| Emergency care | Physical rehabilitation |
| Hospital outpatient care | Preventive care |
| Hearing aids | Smoking cessation services |
| Home health care | Vision care |
| Hospice services | |
| X-rays and other radiology services |
Similar Articles:
- How to Get New York Medicaid Benefits?
- How to Get North Carolina Medicaid Benefits
- How to Get North Dakota Medicaid Benefits
Copayments?
They do not have to pay a copayment; when a member is:
- under 21 years old;
- pregnant;
- Held by the state
- Placed under government supervision
- Native American participants who qualify for Contract Health funding
- Services or Tribal Union of Indian Health Services
- Residing in one of the facilities listed below and funding a portion of their care:
- The hospital (inpatient)·
- A facility for skilled nursing
- A nursing home
What is not covered by Montana Medicaid?
Medicaid does not provide coverage for private podiatrists, chiropractors, naturopaths, psychologists, or therapists (physical therapists, audiologists, or speech therapists).
Medicaid is not obligated to pay for personal care services or nursing supplied by a family member. Bandages, adult diapers, and other disposable items are frequently excluded from coverage, as well as cosmetic surgery and other elective procedures.
How many types of Montana Medicaid are there?
Medicaid benefits are split into two categories: required and elective. By federal law, adults who qualify for Medicaid must receive these services unless exempted under Section 1115 of the Social Security Act. The Montana Medicaid plan gives extra benefits that not all participants can get.
Medicaid Eligibility
What is the highest income limit for Montana Medicaid?
The resource and income standards for Montana’s Medicaid for Workers with Disabilities (MWD) program are significantly higher than those of many other Medicaid programs, at $15,000 for a person and $30,000 for a couple, with a countable income ceiling of 250 percent of the federal poverty level (FPL).
How much money can you have in the bank on Montana Medicaid?
For this program, the maximum asset limit is $2,000 for a person and $3,000 for a pair. Study up on the medically needy route. Asset Spend Down – Seniors with assets above the MT Medicaid cap may “spend down” their assets to become asset eligible.
Does the disabled person get Montana Medicaid?
Medicaid clients working disabled may be eligible for Montana Medicaid for Workers with Disabilities (MWD) program, provided they contribute financially.
Will you still have Montana Medicaid once you are over 18?
A person is at least 18 years old, has a household income between 0 and 138 percent of the federal poverty level, and is qualified for or enrolled in the program.
Similar Articles:
- How to Get Ohio Medicaid Benefits | Best Answers
- How to Get Oklahoma Medicaid Benefits | Best Answers
- How to Get Oregon Medicaid Benefits | Best Answers
What documents do I need to apply for Medicaid?
- The following papers must be included with the application.
- The Social Security Number;
- Evidence of citizenship or authorized residency in the United States, such as a passport, driver’s license, birth certificate, green card, or job authorization card
- Evidence of all income sources, both legal and illegal
- Proof of origins
- Proof of residency
- Including the Medicare card, any insurance cards
- Pregnancy (doctors’ certification of the pregnancy and, if applicable, the expected delivery date);
- When non-parents apply for Medicaid on their behalf, they must provide proof of their financial position.
